What Does a Psychiatrist Actually Do for Depression?
Depression affects over 280 million people globally, says the World Health Organization. It’s a serious medical issue, but one that can get better with proper help. That’s where a psychiatrist comes in.
A psychiatrist is a medical doctor. As medical doctors, we look beyond just ‘the blues.’ When you sit in my office, my first task is to rule out physiological mimics, like a sluggish thyroid or a severe Vitamin D deficiency, that can masquerade as clinical depression.
Once we’ve cleared the physical hurdles, we co-create a roadmap that balances medical intervention with your personal lifestyle goals. Curious how psychiatrists guide people through this? Continue reading.
Key Takeaways
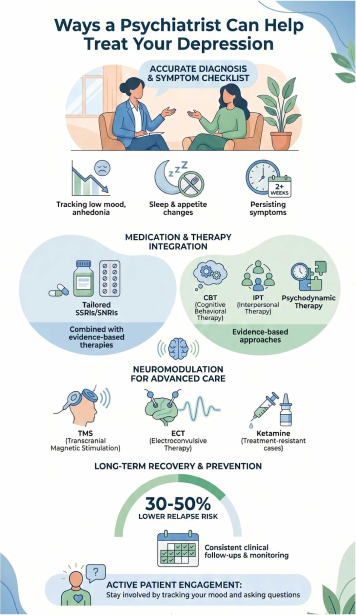
- Psychiatrists use several methods together rather than relying on one approach and build a treatment plan based on symptoms, history, and medical data.
- Many studies suggest that a large proportion of patients improve with appropriate treatment, with some estimates ranging around 70–90% when care is well-managed, though exact figures vary.
- Treatment may include therapy, medication, and brain-based interventions.
How Do Psychiatrists Diagnose Depression Accurately?
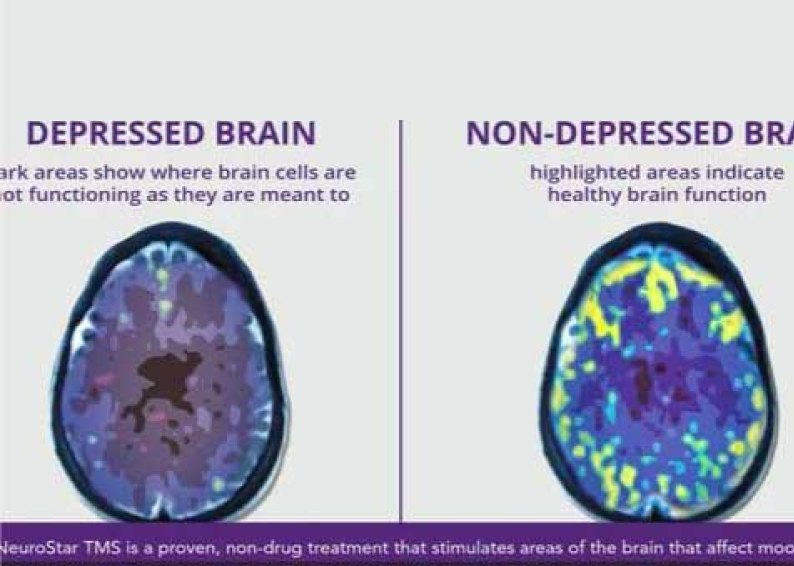
A formal diagnosis isn’t a snapshot; it’s a mosaic. I don’t just look for sadness; I look for ‘anhedonia’, that specific, heavy loss of interest in things you used to love. To make our first session most effective, I recommend patients bring a ‘mood map’ or a simple list of how their sleep and appetite have fluctuated over the last 14 days
These are not casual chats. To figure out if someone has depression, a psychiatrist doesn’t just go by a hunch. They ask a lot of specific questions.
They’ll want to know about your mood, of course, but also your sleep, appetite, energy levels, and how you’re getting through your normal day. For it to be considered clinical depression, those core symptoms, like a crushing low mood or losing all interest in things you used to love, need to have been hanging around for at least two weeks straight.
They often use a standard diagnostic guide such as the DSM-5, alongside other systems like the ICD-11, to ensure consistent criteria. In many cases, structured assessments are also supported by tools used in services such as a Psychiatric Evaluations In Raleigh.
It lists the official criteria, which cuts down on confusion and helps make sure two different doctors would come to the same conclusion.
A big part of the check-up is making sure it’s not something else. Problems with your thyroid, or not having enough vitamin D or B12, can make you feel exhausted and down, just like depression. They’ll usually start with some basic blood tests or ask you about your physical health. That’s to make sure something else isn’t causing the problem.
Before making a diagnosis, the psychiatrist will put together a full picture by looking at a few key things:
- How long the symptoms have been going on.
- How intense they are, are you just feeling blue, or can you not get out of bed?
- Whether depression, anxiety, or bipolar disorder runs in your family.
- If you’re also dealing with signs of another issue, like constant anxiety.
Taking all this time and being thorough is how they avoid getting it wrong and calling it depression when it’s actually something different.
How Does Medication Management Improve Depression Symptoms?

Medication can help, but it is not a one-step solution. Psychiatrists adjust treatment over time based on how a patient responds.
Antidepressants aren’t ‘happy pills’; they are chemical stabilizers. Most focus on boosting serotonin (the ‘mood’ messenger) or norepinephrine (the ‘energy’ messenger).
In my experience, patients see the best results when we find the right dosage that provides relief without the ’emotional blunting’ some fear. Common options include SSRIs like sertraline and SNRIs like duloxetine.
Clinical studies suggest that roughly 60–70% of patients may experience meaningful improvement when antidepressants are carefully chosen, dosed, and monitored over time, especially in cases where depression is formally diagnosed and treated as a clinical condition like Depression Treatment In Raleigh.
That phrase matters. Management involves regular follow-up, not a one-time prescription.
Psychiatrists typically:
- Start with a standard medication
- Adjust the dose based on response
- Switch medications if needed
- Combine treatments in some cases
They also watch for side effects. If a medication causes fatigue, nausea, or sleep issues, adjustments are made. This process can take weeks or months.
Medication works best when combined with therapy and daily habit changes. It supports the brain, while other approaches address thoughts and behavior.
What Types of Therapy Do Psychiatrists Provide or Recommend?
Therapy is a huge part of beating depression. Your psychiatrist might handle it, or they could refer you to a therapist who specializes in certain methods. Many people first get guidance after understanding When To See A Psychiatrist.
As the American Psychological Association highlights,
“The big takeaway is that there are effective options available to treat people with depression” – American Psychological Association
Cognitive Behavioral Therapy (CBT)
CBT is all about your thoughts. It helps you notice when you’re being really hard on yourself in your own head. You figure out how to pause when a harsh thought pops up. You look at it and ask, “Is this really the whole story?” Then you work on replacing it with a thought that’s fairer and a lot less mean.
CBT gives you tools to question those thoughts and swap them for something more balanced and true. Research has found that learning CBT skills can really help lower the chance of depression coming back, which is especially important if you’ve had several episodes.
Interpersonal Therapy (IPT)
IPT zeroes in on your relationships. Problems with people, big fights, a painful loss, or just feeling alone, can fuel depression. This kind of therapy helps you get better at dealing with those things. It aims to improve how you communicate and cope with stress in social settings.
Psychodynamic Therapy
Psychodynamic therapy looks at your past. It uncovers old patterns that drive your current moods. While this ‘deep dive’ provides great self-awareness, clinical data shows that CBT and IPT often work faster for relieving active depression symptoms.
No matter which type you look at, one thing keeps coming up. Structured sessions with clear goals tend to help more than unstructured conversation. Patients often respond better when therapy includes practical exercises.
What Happens When Standard Treatments Don’t Work?
Not everyone responds to first-line treatment. Some research estimates that up to about 30% of people may experience treatment‑resistant depression after one or more antidepressant trials.
In these cases, psychiatrists may recommend advanced options such as TMS therapy for treatment-resistant depression. One example is transcranial magnetic stimulation (TMS). Besides the usual pills or talk therapy, there are other ways to go. They work differently.
TMS (Transcranial Magnetic Stimulation)
For this one, a doctor puts a magnetic coil on your head. It sends magnetic pulses into specific parts of your brain. These pulses are painless. The goal is to stimulate the brain areas that manage mood.
ECT (Electroconvulsive Therapy)
It’s got a bad image from old films, but it’s not like that anymore. Today, you’re asleep under brief anesthesia. Doctors use a small, controlled electric current to trigger a short seizure in the brain. ECT is one of the most effective treatments for severe or life‑threatening depression, particularly when other options have failed or when rapid response is critical.
Ketamine-Based Treatments
This uses a low dose of the drug ketamine. You get it through an IV drip or a nasal spray in a doctor’s office or clinic. For people whose depression hasn’t responded to other treatments, it can start to work in just hours or days. That’s a lot faster than standard antidepressants, which can take weeks.
As published in The American Journal of Psychiatry, rapid-acting interventions have shown meaningful efficacy for patients who have not responded to multiple standard antidepressants:
“In this trial involving patients with treatment-resistant major depression, the use of esketamine plus an antidepressant was more effective than the use of an antidepressant plus placebo.”– American Journal of Psychiatry, 176(6), 422–424.
How They Stack Up
| Treatment | What it is | Used When | Things to Know |
| TMS | Magnetic pulses to specific brain areas. | After several antidepressant meds haven’t worked. | No anesthesia needed. Done as an outpatient visit. |
| ECT | Controlled electrical brain stimulation. | For severe, urgent, or medication-resistant cases. | Very high success rate. Requires brief anesthesia. |
| Ketamine | Low-dose medication under medical supervision. | For treatment-resistant depression. | Can work extremely quickly for some people. |
These aren’t the first things doctors try. A psychiatrist will only suggest them after going through your full history, weighing the risks, and seeing how other treatments have worked for you.
Why is Ongoing Monitoring Critical for Recovery?

Depression changes over time. Symptoms may improve, return, or shift in form. You need check-ins to actually see how things are going. Research indicates that consistent follow‑up care can significantly reduce the risk of setbacks, with some studies suggesting a reduction in relapse risk of roughly 30–50% compared with less structured care
Those regular appointments aren’t just a formality. That’s when your psychiatrist does the real work of fine-tuning your plan. They’ll look at how your symptoms have shifted, tweak your medication or therapy approach, and check in on how you’re actually managing day-to-day life, not just asking “how’s your mood.”
Sometimes they’ll also loop in your therapist or another doctor to make sure everyone’s on the same page, especially when care includes structured neuromodulation approaches.
Getting better isn’t something that just happens during the appointment. The work you do between sessions, and the support system you have in place, are what really build the foundation for recovery.
Why Some Treatments Feel Ineffective
Treatment does not always feel smooth. Many patients report gaps between what they expect and what actually happens in care.
Therapy getting stuck on repeat is a real problem. It’s when every session starts to sound like the last one. You talk about the same things, but nothing really changes or moves forward. That feeling of being stuck in a loop, where you’re just rehashing stuff without getting anywhere new, can make the whole point of going feel pointless.
Others feel that medication becomes the main focus, while practical coping tools receive less attention.
Treatment‑resistant depression affects a meaningful portion of people, which can help explain why many patients feel frustrated when multiple treatments take time to work. Progress can feel slow sometimes, and that’s tough. When things aren’t moving or don’t make sense, it’s normal to start wondering if the whole process is even working.
People often share these specific frustrations:
- The sessions start to feel like a broken record, covering the same ground without feeling personalized to you.
- There’s a lot of talk about medication, but not enough conversation about other ways to cope or what those meds are actually supposed to do for you.
- You walk out the door after an appointment and realize you don’t have a single concrete thing to try before the next one.
These aren’t small complaints. They’re completely valid. Research shows better outcomes when treatment combines medication, therapy, and active patient involvement. Psychiatrists who adjust their approach and include patient feedback tend to see stronger results.
How to Get the Most out of Your Psychiatrist
To truly understand How Psychiatrist Help With Mental Health, recognize that treatment works best as a two-way process. A psychiatrist brings medical expertise, but the patient brings daily experience.
Simple habits can improve how effective care becomes.
- Keep a short record of mood, sleep, and energy levels
- Report side effects clearly, even if they seem minor
- Ask direct questions during appointments
Examples of useful questions include:
- What is the goal of this treatment?
- How will we measure progress?
- When should we adjust the plan?
Studies suggest that patients who stay engaged in their care see better outcomes. Clear communication helps psychiatrists make better decisions, based on real patterns rather than guesswork.
When Progress Feels Slow, Keep Moving Forward
You follow the plan, show up to sessions, and still have days where everything feels heavy and stuck. It’s frustrating. Real progress takes time.
If standard treatments haven’t moved the needle, you aren’t out of options. Modern neuromodulation, such as Medpsychnc, offers a non-drug alternative by stimulating mood-regulating circuits in the brain. While I recommend discussing this with your primary care team first, specialized clinics, including regional centers like Medpsychnc, can provide the specific evaluation needed for this technology
FAQ
Can cognitive behavioural therapy help change negative thoughts?
Yes, cognitive behavioural therapy helps identify and change negative thoughts. It teaches practical skills to replace unhelpful thinking with more balanced views. A mental health professional guides this process. It is one of the most effective psychological treatments for improving mood and daily functioning.
How does Psychodynamic Therapy support long-term mental illness care?
Psychodynamic Therapy helps people understand how past experiences affect current behavior and emotions. It builds self-awareness and improves emotional control. This therapy treatment supports long-term recovery and works well with other psychological interventions in a structured treatment plan.
What is Mindfulness Based Stress reduction in mental health services?
Mindfulness Based Stress reduction teaches focus on the present moment without judgment. It helps reduce stress and improve emotional balance. Many mental health services include it as part of a treatment plan to support better sleeping patterns and reduce anxiety.
When should someone use a crisis hotline or support group?
A crisis hotline or support group can help during intense distress or when support is not available. These options provide quick mental health support and guidance. They help reduce isolation and work alongside care from a healthcare provider or other therapy treatment.
References:
- https://www.apa.org/monitor/2019/09/ce-corner-depression
- https://ajp.psychiatryonline.org/doi/full/10.1176/appi.ajp.2019.19040423